Music is hugely important in my writing process, and I wanted to invite you to listen to “Time” by Pink Floyd in conjunction with this essay. My husband and I heard this on the way to the hospital one day, and it’s been bouncing around in my head ever since.
I’ve been thinking a lot about quantification recently.
This is likely because, for the past nine days, I have been inside a hospital for at least eight hours every day. There is perhaps no place that relies so much on the quantification of human life as the hospital. While I was an inpatient, nurses came to take my vital signs every few hours. Four pieces of quantifiable data told them whether or not I was well: heart rate, oxygen saturation, temperature, blood pressure. And that was all after labor and delivery, during which I was constantly being monitored in order to chart the frequency and duration of my contractions, and my baby’s heart rate was monitored to determine her general well-being.
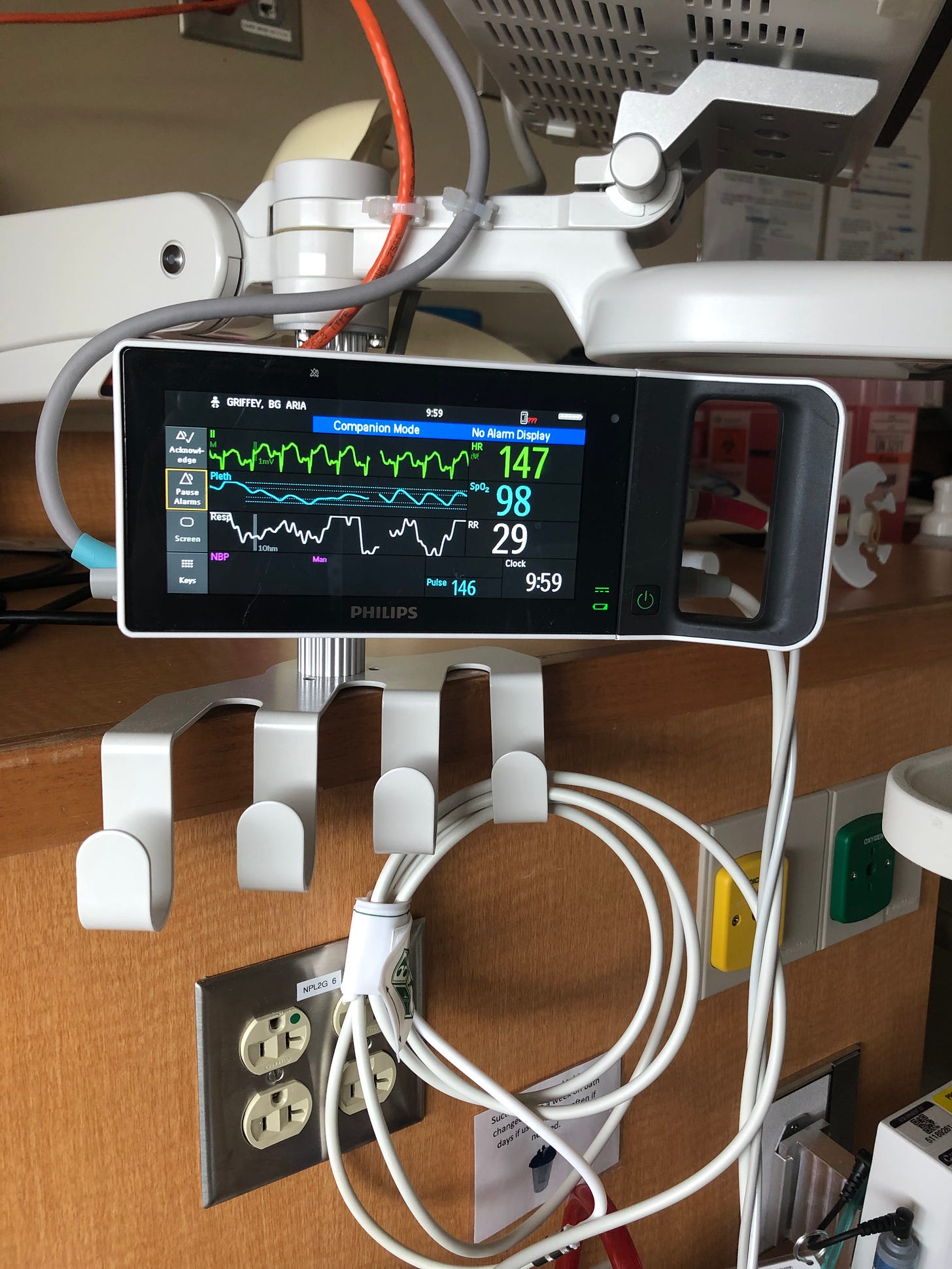
Even now that labor and delivery is over, the quantification of my daughter continues even more intensely. In the neonatal intensive care unit, she is monitored constantly for her heart rate, oxygen saturation, and respiratory rate. These three data points print out in neat colored lines on a digital display angled so that we can always see it from the bedside, even when we cannot see her so clearly. Every diaper she soils is weighed and charted, every feed measured out in milliliters from the plastic capsules of pumped milk I bring from home. They measure the percentage of pressurized oxygen they are constantly pumping into her lungs through the little nose mask that looks like it belongs to the world’s tiniest scuba diver; 30% and then 28%, then up to 40% for short periods of distress which cause her oxygen saturation to drop dangerously. The goal is 21%—room air levels—but it hovers deceptively far away.
In search of comfort, I too turn to quantification: I religiously track milliliters of milk pumped, scribbling them down to assure myself that yes, I am producing enough to feed my daughter, even though that feeding happens from a syringe pumped into a feeding tube that runs down into her stomach via her nasal cavity. I track how many times a day I “kangaroo:” hold my daughter skin-to-skin on my chest in order to regulate her heart rate and temperature. A poster on the wall touts the benefits of this practice and encourages me to “ask my nurse about kangaroo care today!” I try not to think about the fact that I must ask a nurse every time I wish to hold my daughter, nor the fact that when I do hold her, it feels like half of what I’m holding is just lifeless medical equipment—tubes and wires and electrodes hanging off her tiny body like tentacles.
When I talk to others about my labor and delivery, I can’t help but try to quantify my experience: 6 bags of penicillin, 3 bags of saline, an unknown quantity of Pitocin that at one point caused me to throw up between every contraction, 24 hours they think my water was broken before I was admitted (I suspect it was longer, but I never told the nurse for fear they would take my treatment to even further extremes), the eight or so hours it takes to dilate from 4 to 5 centimeters, and the endless agony I spend at 5, never seeming to get any further even as they turn up the Pitocin higher and higher. The numbers feel solid, something to grasp in the shapeless 22 hour muddle that is the time from my admission to my daughter’s birth at 12:42am on Friday the 17th of May.
I scan the visit notes from nurses and doctors in my online chart, looking for more numbers, more crumbs of data to help me understand the experience. I find the existence of the notes, time stamped and arranged chronologically, strangely comforting; they solidify my experience as a Real Thing, observed and documented by others, a quantifiable chunk of time I spent a certain way.
Since then, time has become a slurry, hours in the postpartum ward and the NICU and eventually home bleeding into one another until my husband and I can no longer remember what day it is, or whether we fought this morning or yesterday morning, or how many times we’ve eaten lunch in the same chain restaurant within sight of the hospital. Without numbers and data to document it, this shapeless mass of time feels unreal and incommunicable, a shared hallucination destined to last until the day we bring our daughter home.
Whenever I’m looking for a healthy injection of tech skepticism, I like to read
’s Substack . I found myself catching up yesterday while I pumped milk at the hospital; thanks to an $11 hands-free bra, perhaps my best purchase since the birth of my daughter, I can now perform basic tasks like writing emails and scrolling Facebook while pumping, which is immensely freeing after days of holding pump parts by hand every three hours. His recent post about the 2024 Consumer Electronics Show makes me want to throw my cellphone across the NICU ward.“If the metaverse is here to cover our eyeballs with digital worlds, then the Internet of Things and the Internet of Bodies are set to cover our physical world with digital eyeballs,” Allen writes.
“…our bodies are to be watched by wearables or even implants—our heart rates and our emotional states, our digestion and our sexual arousal. We are to become data.
Companies like Body Log, SensePlus, and SmartSound AI can measure every process in your brain and body like barely visible, but overly curious nurses. For those who want to continue their bloodline into this dystopian web, products like Sperm Tester are there to make sure your boys are swimming straight. The Louise app—named after the first baby conceived through in vitro fertilization in 1978—was created to identify the causes of infertility in the hopes of finding an appropriate workaround. Once your baby is born, companies like HubDIC can provide an IoB crib outfitted with a moving camera to monitor the infant’s every move and whimper.”
One of the photos shows an example infant in the aforementioned digital eyeball crib, whimpering plaintively as it lies on a wire-bedecked pad, perhaps designed to capture the baby’s vital signs as it sleeps. I feel like vomiting. I genuinely restrain myself from throwing my phone across the room, because it feels like just another piece of this evil data machine (it is.)
I imagine an anxious parent purchasing the massive isolette that currently holds my daughter and willingly placing their healthy newborn inside, hooked up to wires and probes and monitors that feed into their phone 24/7, assuring them that their baby is healthy and safe and getting enough oxygen. I imagine said parent sitting in a sweetly decorated nursery at home next to the comically large isolette, staring at the numbers on their phone while the baby lies inches away, wiggling and begging for love and attention. I imagine said parent reassuring themselves that baby is safest being monitored and quantified, because if something is wrong the app on their phone will beep, informing them of a drop in oxygen or a sudden spike in heart rate. Maybe there is a subscription service for an around-the-clock nurse to monitor and perform cares while the parents are at work. “Now you never have to worry about your precious little one again,” says the jaunty advertisement, “Just open the app on your phone and see your baby’s stats 24/7, at the office, during your commute, or even from the next room.” Even from next to the crib.
I imagine the next generation of the Safe Sleep campaign: “ABCs of safe sleep: Always use the App, Big Brother is watching your baby, Caring is Sharing (your child’s data).” Insurance companies are legislated to cover mandatory eyeball cribs. The health department now not only checks to see if your car seat is safely installed, but comes to your home to ensure you’re complying with the new Safe Sleep. Failure to comply may result in a lapse in coverage from the state insurance system, or perhaps removal of your baby by child protective services.
I ponder this grim dystopia while I watch my daughter’s vitals trace across the screen in the corner. In the labor and delivery room, my husband took it upon himself to stop me from obsessively watching my own stats on the monitor, even as I tried to police him from watching himself. “I’m right here,” I said, “Pay attention to me. I’m the one who’s having the contractions, not the computer.” He told me that it was his job to worry about the stats; watching them myself would only worry me unnecessarily.
I missed at what point my daughter’s heart rate began dropping every time I had a contraction, indicating fetal distress. I barely remember a conversation with the nurse, a no-nonsense woman with an incredible bedside manner. She told me that we could try one or two more position changes, but if my daughter didn’t respond then we would have to move to an emergency c-section. Suddenly, I was willing to do anything, to crawl over broken glass to prevent that from happening. I lay on my side even as every contraction sent searing pain through my hip and leg. My daughter responded. We were spared a c-section.
I named this Substack The Unquantified Life because I have grown weary of personal quantification as the path to an actualized self. The health and wellness industry seems bent on convincing us that if we just measured this data point or tracked that macro or used that app every day, we would be transformed into the happier, healthier, more fulfilled selves we desire to manifest. Whether that looks like counting calories, steps, or meditation sessions, the promises are all the same. More data gives us more control and makes us happier.
But I believe that, as Joe Allen writes in the CES article, submitting ourselves to more scrutiny, surveillance, and measurement makes us less and less human. At some point, we will reach a state where the monitors are not supplementary information to help guide care decisions, but rather the final proof of whether anything is happening at all. I experienced this first hand in the postpartum ward, before I was unceremoniously discharged after the 48 hours mandatorily covered by insurance. Nurses took my vitals every few hours, pressed on my belly to see if my uterus was contracting back to regular size, and squeezed my calves, asking if there was any pain that might indicate a blood clot. They also asked my general pain level from one to ten, though always at a junctures when I was lying down and relatively comfortable, thus receiving a deflated answer. Everything measured was completely normal, even very good. So when I tried to explain that I was experiencing shortness of breath and pain in my lungs, constantly but especially when I got up and moved around, I was dismissed out of hand. My vitals were normal, my oxygen saturation at 98%. The problem must not exist because it could not be measured. No one even offered an explanation for the symptoms. They were ignored.
Right before we were discharged, I asked the attending nurse again, determined to be heard, especially since shortness of breath was listed among the severe warning signs on the back of the discharge papers. Finally, I received a potential answer: the nurse said it was likely pain in the muscles around my rib cage, caused by sitting up to push more effectively during delivery. The exertion had strained the muscles in my back and chest, so I was not having pain in my lungs but pain in my ribs. The explanation made total sense, and I accepted it readily. She was the first nurse I’d spoken to in 48 hours to offer any kind of explanation at all.
Despite my concerns and fears about the proliferation of monitors, data, and quantification, in this instance I find myself afraid their absence. When I am finally able to try nursing my daughter, I immediately fear she is not getting enough milk. There is no way to directly measure how much she is actually consuming at the breast1; bottles come with handy markings in ounces and milliliters, and so do feeding tubes. The only way to reassure myself is through indirect signs: her weight gain, her diaper count, her body language. Soft, malleable, subjective things, the opposite of hard data. How much more convenient, more reassuring, to have precisely measured milliliters of milk drained gently through a feeding tube into the stomach. But my daughter knows this is not the right way. She pulled her feeding tube out twice before they decided she was taking enough by mouth that it no longer mattered. She is much happier without it.
The numbers on the monitors are reassuring also; if my daughters oxygen or breathing rate dip too low, a chime will sound and trained nurses will rush to her bedside. When she comes home, this will not be the case. I think about SIDS and all of the Safe Sleep campaigns. I fear that, without the constant monitoring, my daughter will stop breathing, or suffocate, and I will never know until it’s too late.
There is reassurance in data; concrete proof that we are not crazy, that our eyes are not lying to us, that there is something there to be measured. Without this data, would I trust my daughter was well, even if I stared at her, watching every breath and move and blink? Would I believe her body and what it is telling me? Would I know what to look for? As a society, we have lost the ability to read the clouds and the stars, the signs of the times, even our own bodies’ signals. Far more interesting distractions prevail. Pics, or it didn’t happen. Data, or how can you prove it. Quantification, or oblivion.
My husband and I were both immensely reassured when, during one of our daughter’s care times, the nurse took her respiration rate the old fashioned way. She put her hands on the tiny body and watched the clock, counting in her head. The action required finesse and focused attention, skills hard to come by in our digital age. The electric monitors are helpful, sometimes even necessary, but they can be rendered inaccurate by displaced wires and a little wiggly body. The fact that the nurse trusted her own senses and observations instead of investing blind faith in the machine only served to drive home the quality of care that my daughter is receiving in the NICU. I am more reassured by this single check than if I had a monitor streaming 24/7 to my phone.
I find myself in the gap between two truths: quantification can be harmful, but also necessary. What starts out as a discrete medical tool can quickly become a catch-all consumer product; my brother visited wearing a smart watch that tracks his own vitals, sleep cycles, and exercise around the clock. No doctor prescribed it to him. He seems to use it out of curiosity more than anything, or perhaps competitiveness.
I would prefer to inhabit my own body, with all its vagaries and subjective cues and slippery experiences, rather than viewing it from the outside through physicians’ tools. I would wish the same for my daughter, for my experience of her. I do not wish it to be mediated this way. But, for now, it is. And I’m trying my best to be okay with that.
Well, disturbingly enough, now there is. This post on
makes an excellent accompaniment to my ponderings here.


Feel all of this so deeply, it is such visceral writing. The techy tug-of-war is impossible and confusing, I so relate— and thanks for the shoutout!